Ticks and Lyme Disease
Guidelines for removal and submission of ticks for identification and possible screening for disease-causing agents
Tick Removal
Ticks are most effectively removed with a fine pair of tweezers (forceps). Grasp the tick with tweezers as close to skin as possible. The tweezers should be held at a right angle to the tick's body. Gently, but firmly, pull the tick up and away from the host's skin. Avoid twisting or turning the tick during removal as this can cause the tick's mouthparts to break off. When this occurs, it is more difficult to identify the tick to the species level and could cause infection at the feeding site. When appropriate, disinfect the feeding site after the tick is removed. Once removed, immediately transfer the tick to a collection vial. Avoid handling ticks with bare hands. Use disposable gloves, paper toweling or tweezers when transferring ticks to the collection vials. After handling ticks, discard gloves and paper toweling and wash hands and tweezers thoroughly.
 |
 |
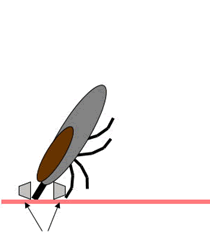
| SIDE VIEW: Position the jaws of the tweezers around the mouthparts of the tick and as close to the skin as possible. |
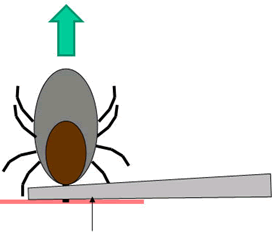
FRONT VIEW: The tweezers should be held at a right angle to the tick’s body. Gently, but firmly, pull the tick up and away from the host’s skin. |
Collection vials, labeling, submission information & storage
A suitable collection vial should:
- be large enough to accommodate the submitted specimen without damaging it;
- be made of rigid plastic (never use glass) to ensure the tick is not damaged during shipment; and
- have a lid or top that fastens securely (the lid can also be taped to ensure the lid is not dislodged during shipping).
Common household containers that make good collection vials include film canisters and pill bottles.
Paper toweling should be placed in the collection vial to cushion the specimen and to maintain the quality of the specimen during shipping Collection vials should be clearly labeled, using a permanent marker, with at least the collector's or submitter's name, the location and date the tick was collected and type of host the tick was removed from (For example, John Doe, Winnipeg, Manitoba, July 1, 2007, host - cat). Depending on the type of collection vial, this information can be written directly on the vial, or on masking tape or a paper label fastened to the vial.
In addition to the label, a submission form Document (PDF document - 766 KB - 1 page) (instructions on how to download) MUST be completed and sent with the specimens. Use of the submission form helps to ensure that all pertinent collection and host information is provided and also informs the laboratory where (and to whom) to report the results of the identification or diagnostic testing. When ticks are collected from different hosts or localities, separate submission forms should be completed.
Prior to shipment, ticks (live or dead) can be temporarily stored (within the collection vials), for 7 to 10 days, in a refrigerator. If collected ticks appear to be dead, based on a lack of movement, or they cannot be shipped for several weeks, they can also be stored in a freezer, as this will prevent mold from degrading them. If one does not have access to a refrigerator or freezer for several days, ticks in collection vials should retain their quality at room or out-door temperatures. However, consider placing ticks in 70% alcohol (isopropyl or rubbing alcohol is suitable) if they have to be maintained at room temperatures for longer than 5 days. Storage in alcohol should not affect the ability to test submitted ticks for disease-causing agents. Regardless of the method of storage, collection vials can be shipped without any further preservatives such as cold packs or dry ice.
Shipping instructions
Place collection vials in a Transport Canada approved mailing container (or a larger specimen container or cardboard box). To minimize breakage, support the collection vials in the mailing container with bubble pad, packing chips or paper towel. Use an envelope or plastic bag to protect the submission form(s) and do not forget to put them in the mailing container with the submitted ticks. Seal the mailing container with masking or adhesive tape.
Ticks can be shipped using local courier companies (e.g., FedEx, Purolator, Greyhound, Priority Post, etc.) or through Canada Post (regular mail service). Though regular mail is likely the most inexpensive way to send specimens, this method typically takes much longer than courier services and delivery is not guaranteed. The urgency and relative importance of having a collected tick identified and tested should be considered when selecting the most appropriate shipper (i.e., ticks from people compared to ones from wildlife or livestock).
When possible, ticks should be sent to provincial collaborators who will identify the tick and then forward only the blacklegged ticks to the National Microbiology Laboratory (NML). The NML will conduct diagnostic testing for the Lyme disease agent as well as several other disease-causing agents.
Please note that it usually takes at least two weeks for ticks submitted to the NML to be identified, tested, and for results to be reported to the original submitter. During the peak periods of adult tick activity (October to December), the processing time at the NML can extend to 4-6 weeks because of the large volume of tick samples received.
For information on where to send tick specimens in your area, contact the NML through phone or email at:
National Microbiology Laboratory
Phone: (204) 789-2000
Email: ticks@phac-aspc.gc.ca

To share this page just click on the social network icon of your choice.